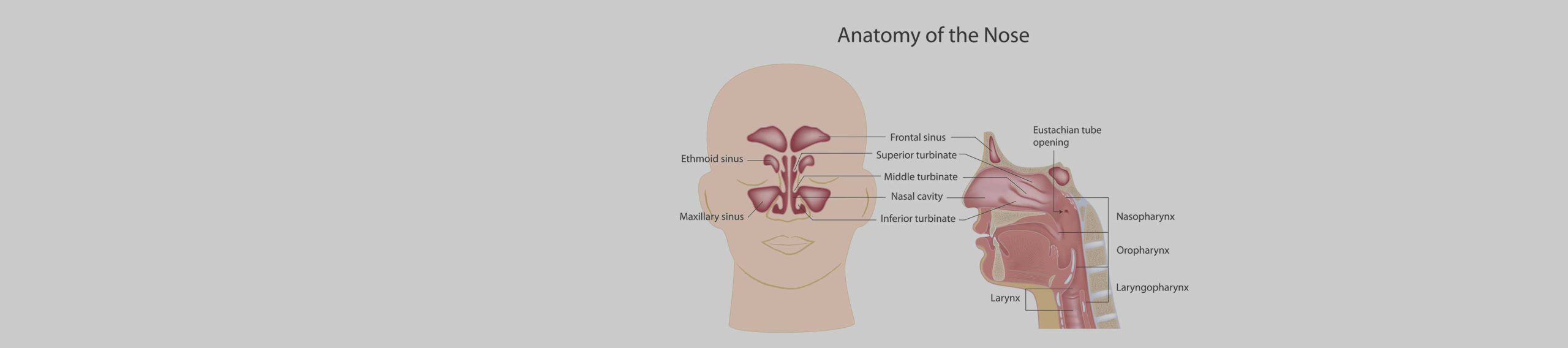
Sinusitis
Acute sinusitis is a viral or bacterial infection of one or more of the sinus cavities which are normally air filled spaces in the skull. People with allergies are predisposed to sinusitis because of ongoing nasal inflammation, which impedes the normal drainage of the sinuses into the nose via small openings.
Obvious or subtle symptoms can occur with sinusitis. These can include fever, chills, headache, pain in the face and upper teeth, nasal congestion, decreased sense of smell, mucus in the throat and nose, and cough. In some cases, patients may experience only nasal congestion, mucus drainage in the throat (post nasal drip), bad breath (halitosis) or recurrent coughing, especially at night. Some patients with asthma will note worsening of their wheezing with sinusitis.
Chronic sinusitis is a complex disorder with many triggers: allergy, inhalation of irritants (such as tobacco smoke), scarring from previous infections, or anatomic abnormalities like a deviated septum or nasal polyps. People with chronic sinusitis do not always need antibiotics, though sometimes they are necessary if there is an acute bacterial flare-up.
Treatment of sinusitis depends on the nature of sinusitis, i.e. acute or chronic, viral vs bacterial, etc. For chronic sinusitis, the first step is allergy testing to see if environmental allergies are driving your ongoing sinusitis, as this information will also help guide treatment. But, daily saline irrigation is the basis for treating all subtypes of chronic rhinosinusitis. Topical decongestant sprays and inhaled nasal steroids sprays may also help to promote better drainage. In some cases, a short course of oral steroids can be used to decrease inflammation and promote drainage. Of course, antibiotics are also used when necessary. Sometimes a CT scan is also necessary especially if an anatomic cause is suspected.